Martial Arts will leave you black and blue but we love it and here you’ll read about the most common injuries we see amongst fighters including some input from Australia’s most decorated fighter and all round top bloke John Wayne Parr.
Tennis Elbow: Getting to Grips with the issue
About:
Tennis elbow is a very common term used to describe lateral elbow pain. However, people can experience the condition without having ever picked up a racquet. The most up to date term currently is lateral epicondylalgia (LE) with “algia” meaning pain. This reflects the general shift away from it being considered an inflammatory condition in which the tendons around the elbow are inflamed. Rather, it is thought that the tendons become overloaded and sensitisation of the area occurs causing a heightened pain response that in turn causes inhibition of the muscles in the forearm. Inhibition results in a decrease in muscle “strength” which means everyday tasks like lifting a kettle become harder and tend to overload the tendons further causing more pain which causes more inhibition etc. (a vicious cycle of pain).
Even though the area of pain is usually focused around the outside of the elbow, it is actually the tendons of the forearm and wrist muscles that are affected. They come from a common origin point which attaches to the lateral epicondyle of the humerus bone. The implications of these tendons/muscles being affected is that it is mainly wrist and hand movements (e.g. gripping and lifting) and not elbow movements that are most painful.
Usually tendon pain occurs either through an acute injury or abnormal loading of the tendon (e.g. awkward tennis swing or a repetitive task at work). However, LE can also occur with no specific trigger. Around 40% of people will experience some form of LE in their lifetime and it is most prevalent those aged from 35-54 years (Bisset & Vicenzino, 2015). Regardless of the cause, it can be treated successfully to return the sufferer to full function. This will usually involve a loading program for the tendons to gradually improve their capacity and to “re-strengthen” the muscles. Rest alone does not address the muscle weakness or drop in capacity and this results in prolonging the injury. Weakness around the shoulder blade and shoulder muscles also needs to be addressed as the elbow can be the point of compensation for those areas further up the chain.
Common presentation:
· Pain in the lateral elbow or into the forearm
· Pain with tasks like lifting and gripping
· Weakness with tasks like lifting and gripping
General advice:
· Ice over the painful area (usually lateral elbow)
· Massage the forearm muscles (NOT the lateral elbow)
· Avoid poking or prodding the painful area (feels good at the time but really tends to make it worse)
· Use of a brace or taping around the upper forearm
· Avoid aggravating activities
· See your physiotherapist for a gradual loading program
· See your physiotherapist for an upper limb strengthening program
It is always best to be assessed by a physiotherapist to ascertain a correct diagnosis so you can receive the best treatment possible for your specific condition. Here at East Vic Park Physiotherapy, our physiotherapists are very experienced in assessing and treating lateral elbow pain. Click the link at the top of the webpage to book an appointment or call us on 9361 3777.
References:
1. Physiotherapy management of lateral epicondylalgia. Bisset, L & Vicenzino, B. 2015. Journal of physiotherapy (61), 174-181.
AC Joint pain - The "Other" Shoulder Pain
Anatomy
The Acromioclavicular (AC) joint is located at the lateral tip of the shoulder. The joint is formed by two bones, the clavicle (collarbone) and the acromion (a portion of the scapula/shoulder blade). In between the joint sits a fibrocartilage meniscal disc and the bones are connected by a number of ligaments, muscles and a joint capsule.
Role
The AC joint acts as a pivot point in the shoulder allowing the shoulder blade to rotate as the arm is lifted upwards. If it is dysfunctional it affects the control of your shoulder.
About
The AC joint is very commonly injured in contact sports that involve tackling like rugby or AFL. This is classified as a traumatic injury in which the ligaments can be torn and the capsule disrupted which results in the bone separating. However, you can also have AC joint pain from overloading the joint or degeneration of the fibrocartilage meniscus. It can also develop into a condition called osteolysis which is quite common in gym goers.
Differentiation from “bursitis” or impingement (common shoulder pain)
Shoulder bursitis/impingement is a very common condition in which the bursa and tendons in the shoulder get inflamed or overloaded. Often a cortisone injection is prescribed which can reduce the pain if the bursa is the main issue. However, if it is not the correct diagnosis then ongoing pain and disability can perpetuate. It is very important to get your shoulder assessed by a physiotherapist to differentiate between the two conditions so the right treatment plan can be selected. Please note that Impingement CAN occur as a result of AC joint pain or injury but is not the primary diagnosis.
Common presentation
· Pain at the top or tip of the shoulder
· Difficulty lying on the shoulder
· Difficulty bringing the arm across the body
· Pain with lifting an object above your head
· Pain with gym activities like bench press
General advice
· Try icing the area especially when it is painful
· Rubbing voltaren gel on the area can help reduce pain, the joint is superficial enough for the gel to have some effect
· Applying taping to pull the shoulder upwards can take the pressure off the joint and relieve discomfort
· A structured rehab program is helpful in making the muscles around the joint stronger so there is less load on the area
· A cortisone injection can be helpful if conservative treatment isn’t effective, as long as they inject the right spot
· Most importantly, visit your highly trained physiotherapist for a thorough assessment and in-depth treatment plan
THE IMPORTANCE OF MUSCULOSKELETAL SCREENING
Finals time for most winter sports is fast approaching and from a physiotherapy perspective this is the time of year that we see a spike in sporting injuries. A lot of these injuries tend to be to parts of the body that have some sort of deficit, be it strength, length or control. It is quite hard to be able to identify these areas yourself and even physiotherapists would find it hard to accurate identify these deficits purely through observation.
Plantar fasciitis
WHAT IS IT?
Plantar fasciitis Is a very common cause of heel pain. It can be quite debilitating and can last for months if not addressed. Typically, pain will be felt on the inside of the heel and arch. Pain can be sharp or achy. There can be a small amount of swelling over the medial heel as well as tenderness to touch. Mornings are worse, with it usually taking anywhere from 2-3 minutes to an hour for the stiffness and pain to reduce.
POSSIBLE CAUSES
· Change in load eg Running/jumping
· Change in footwear
· Change in activity surface eg. Hard surface
· Acute trauma eg. Stepping on a rock
SCANS
Sometimes your GP will refer you for a scan of the affected area. Most likely it will be an x-ray or an ultrasound. This may show that there are heel spurs or “tears” in the plantar fascia. Although it can be good to confirm the diagnosis, scans can sometimes be detrimental as it may cause people to become worried about their condition. Scan results can also correlate poorly with symptoms an example being that people with heel spurs on x-ray don’t necessarily develop Plantar fasciitis.
TREATMENT OPTIONS
· Soft tissue release
· Joint mobilisations
· Taping techniques
· Orthotics
· Exercise program (Physiotherapist prescribed)
· Load management plan (Physiotherapist prescribed)
LOAD MANAGEMENT
Load management is about controlling how much you use the particularly area on a day to day basis. Usually when an area becomes painful, its load capacity (ability to tolerate load) is reduced so it becomes overloaded quicker than normal. This means that even normal tasks or activities like walking or standing can cause it to become more painful and swollen.
One of the ways to improve the capacity is to progressively build up the amount that you use that area. This can be done with a specific structured exercise program (physiotherapist prescribed) that is made more difficult over a period of time. It is normal for rehabilitation to be painful, you cannot improve load tolerance without causing some discomfort.
The best way to monitor improvement is by recording morning pain (rating it out of 10, 10 is worst, 0 is nothing). It is normal to have ongoing morning stiffness even after pain has completely disappeared.
DIFFERENTIAL DIAGNOSIS
Sometimes Plantar fasciitis might not be the cause of heel or foot pain. It is important to see a physiotherapist to get an accurate diagnosis. Other causes of heel pain are below:
· Plantar or Calcaneal Nerve pain
· S1 radiculopathy
· Stress fracture
· Tarsal tunnel syndrome
· Fractures
· Retrocalcaneal bursitis
· Spondyloarthropathies
· Cancer (osteoid osteoma)
TIPS FOR PAIN FLARE UPS
· Try to avoid walking around in bare feet
· Using ice over the sore area can give temporary relief
· Stretching it may be uncomfortable so roll a golf ball/tennis ball under the foot instead to release tight muscles
· Pain relief or anti-inflammatory medication can be helpful but ask your pharmacist for advice
· See your physiotherapist for a progressive loading program
Groin Pain
As pre-season training gets underway for winter sports codes we generally see an increase in the number of patients with groin pain presenting to our clinic. Discussing groin pain as a whole is a very large topic, so for the purposes of this blog I will discuss non-traumatic groin pain and in particular the most common factors that can lead to injury.
Non-traumatic groin injuries are typically complex and require a thorough assessment to determine the factors that have led to the injury and a comprehensive exercise rehabilitation program to recondition the athlete to be ready to return to their sport.
WHAT IS IT?
Groin pain is an umbrella term for pain felt in the groin area. It is not diagnostic and does not indicate a specific pathology or tissue(s) affected. Groin pain can be sub-grouped into 6 different areas:
· Adductor related
· Hip flexor (iliopsoas) related
· Abdominal (inguinal) related
· Pubic related
· Hip joint related
· Other (neural, referred pain, fractures, abdominal/gynaecological conditions etc)
It is common more than one of these sub-groups to be affected and insufficiencies in one area can lead to an overload in another.
WHY DOES IT OCCUR?
Three common reasons for the development of groin pain in sporting people include training errors, poor mechanics and age.
· Training errors causing injury usually refers to “too much too fast” and is usually seen with athletes rapidly increasing their training amounts without adequate recovery between sessions causing a progressive overload of structures in the groin area. Groin pain will commonly present as preseason training reaches 3-4 weeks in and more commonly as running demands transition into higher amounts of sprinting and agility.
· Poor mechanics refers to muscle imbalances, poor movement control and patterns, poor posture, inadequate strength, lack of flexibility and sub-optimal technique for sport specific skill. This is where a good sports physiotherapist will be able to conduct a comprehensive assessment to determine which of these factors are contributing to your groin pain.
· Younger athletes are more susceptible to developing groin pain as their skeletal system is less mature to withstand the stress that training can put on the body compared to older athletes (25+ years).
MANAGEMENT
The pain will generally settle with a combination of rest and anti-inflammatory medication. During this rest period it is important to address the factors that have led to developing groin pain (poor mechanics) to avoid reaggravating the injury when you return to running. It is very important to have a graduated return to running plan in place to allow for optimal recovery between sessions and avoiding too much load too soon.
PREVENTION
The old adage “prevention is the best cure” is applicable for groin pain and there is plenty that can be done to prevent it. If you have had groin pain in the past, having a preseason screen with your physiotherapist is beneficial to assess if any predisposing factors are present. A comprehensive strength and conditioning program to address any factors as well as condition your body to tolerate the training loads can help prevent groin injuries. Also making sure to optimise your recovery between sessions – for helpful tips read our blogs on recovery – will help prevent the development of groin pain.
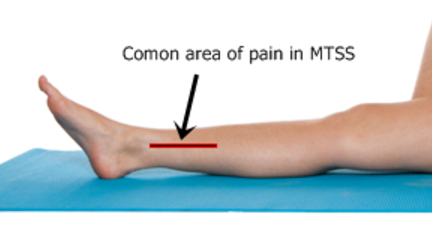
Shin Pain and Medial Tibial Stress Syndrome - An Update
Is there an answer or should I toughen up and suffer in silence?
Preseason is a common time for overuse injuries and pain to present due to the sudden increases in training volume and intensity. Shin splints is one such injury, which seems to just get worse and worse. Often this problem plagues the athlete annually at this time of year. Occasionally it persists into the season to the point where the athlete is constantly playing through pain, suffering post-game and performances can begin to be affected. Since they haven’t had an “injury”, the athlete often feels like they just need to toughen up, push on through and it will pass. However, the problems seem to only get worse and worse the harder they push. Other athletes take time off and are increasingly frustrated to find the injury returns as soon as they get back to business.
So what is shin splints and what causes it?
Shin splints is actually a loose term because it encompasses a range of presentations, including stress fractures and compartment syndrome. It is still widely used but an attempt is being made to oust it. You may or may not have heard your physio refer to it as medial tibial stress syndrome. Medial tibial refers to the inside of the lower shin where symptoms are most frequently reported. Stress syndrome simply indicates that relative overuse is most commonly the cause.
As the narrowest part of the tibia, tiny bending movements occur at this site when running. This causes microscopic breakdown of the bone. There can also be breakdown of the connective tissue that encapsulates the deep muscles of the calf, where it attaches to the bone at this location. However, this is a normal process that occurs in everyone every time they go for a run. The strength of the original tissue and the amount and intensity of the running determines how much breakdown occurs.
Our bodies respond well and adapt to training. Our immune system will usually kick in pretty quickly to clean up the breakdown and lay down new bone and connective tissue in its place. As seen in the picture below, given proper loading volumes and recovery time, our bones overcompensate each time to get thicker, denser and stronger. This means that we can tolerate increasingly difficult challenges. This is a very similar process to how you can build muscle in the gym. However, bone does take a longer to recover, and longer to grow than muscle, but is just as plastic and adaptable.
From "How much is too much? (Part 1) International Olympic Council consensus statement on load in sport and injury risk" by Soligard et al. British Journal of Sports Medicine 2016: 50:1030.
How do I know how much is too much?
This varies greatly from person to person and is dependent of a number of factors.
Loading spikes:
We know that strong bones better resist breakdown and we know that bones get stronger over time. However, if you suddenly increase your training volume, frequency or intensity, you may not have time to sufficiently develop the bony adaptions necessary. Sometimes even changing mode of training to something very taxing on the calf muscles, such as hill running or skipping, is enough of overload the capacity of the tibia. Consistency and gradual increases in training load are imperative to avoid loading spikes.
Strength
Muscles develop at a different rate to bones. Importantly, muscle size is consistently associated with bone size and strength. This means bigger muscles are usually attached to stronger bones. Resistance exercises had been shown to increase bone density. Therefore, calf strengthening exercises can be useful in increasing the strength and size of the tibia so that less breakdown occurs.
Type of Runner
There are two extremes on a spectrum here. There is the athlete with calf and Achilles tendons like Pogo sticks. They often may be lacking in shock absorption and propulsion elsewhere. Naturally, if this is their primary source of power, it will also be the first area to overload. These athletes can often benefit from addressing the weaknesses elsewhere, reducing the demand on the calf muscles.
The other end of this spectrum is the athlete that has weak calf muscles, and is often knee dominant and heavy footed. A change in loading where calf strength is necessary can expose this weakness and cause overloading. Running retraining, and calf strengthening can work well in this population.
Nutrition and Bone Health:
Some people are genetically more vulnerable to low bone density. A family history of osteoporosis or stress fractures may hint at this as a factor. Another key issue is diet. We all know calcium is good for bones but vitamin D is also essential. Under-eating often occurs unintentionally, but when diet is compared with the massive energy requirements of greater than 5 sessions a week, calorie intake often becomes insufficient to meet energy expenditure. Nutrition is key to good bone health, and you can’t outrun a bad diet.
Pain Threshold
Pain is a protective mechanism, like a car theft alarm. It is designed to go off early and loudly before any substantial damage. This is a warning that there may be something to address. However, this threshold is very adjustable and dependent upon a multitude of factors. For example, the local nerve fibers become increasingly irritated and easier to set off when they are repeatedly overloaded. The red line in the picture above moves upwards and so it takes less to set it off. Like a car alarm that goes off in the middle of the night, it seems to get louder and louder.
We also know that lifestyle factors like getting poor sleep, feeling run down, stress, anxiety etc. can lower your overall pain threshold in the absence of pain or injury. In this instance, it takes much less breakdown to fire a pain response. Here, it is vital to address any of these factors that are modifiable to reconfigure the pain threshold to a more reasonable level.
Can the bone fracture?
The overwhelming majority of cases of medial tibial stress syndrome do not lead to stress fractures. This is because the rate of repair and breakdown usually meet an equilibrium long before the integrity of the bone is compromised. However, in some isolated incidences bone stress fractures can occur but this is rare. The pattern of pain with stress fractures is different from medial tibial stress syndrome. If you are concerned about developing a stress fracture, your physiotherapist can quickly establish the likelihood of it.
How do I know if I have medial tibial stress syndrome?
The common description of pain, is a dull diffuse ache along the inside of the shin. It will usually extend at least 5cm along the middle of bottom third of the shin. This pain comes on the beginning of exercise, but will often “warm up” and be less prominent as the exercise continues. As the local tissue becomes more irritated, it will last longer into exercise and may begin to even cause pain after exercise when walking or going up and down stairs. It is not limited to runners, and is very common in footie, soccer, hockey, netball and other field sports.
How long will it take to get better?
Compression garments, massage, dry needling, taping and shoe inserts may offer some short term relief. However, the results are mixed and often require trial-and-error to determine what works for that individual. They won’t solve the problem but can get you through the pain for long enough to successfully adapt.
There is great potential for long-term success the causing and contributing factors are identified and addressed. It can take time to build up the muscular, tendon and bone capacity. Likewise, the nervous system can take some time to cool down, especially the longer it has been wound up. Until then, a certain amount of patience is required. This carefully measured approach is the best way to ensure the problem doesn’t continue to spiral and progress.
What can I do for my shin pain?
1. Catch it as early as possible before it becomes increasingly irritated.
2. Start a training diary to get an idea of how much you are doing and how consistently you are training.
3. Address lifestyle factors if they are modifiable, such as diet, sleep and stress – obviously, this is not always possible!!
4. Visit a physiotherapist to identify your personal contributing factors and develop a management plan – there is no one-size-fits-all approach.
Wrist and Hand Injuries
We use our hands repeatedly every day so it’s not surprising that sometimes we develop pain and discomfort in our fingers, wrists and forearms. Injuries in the wrist and hand can be caused due to traumatic events (e.g. a fall on an outstretched hand) or overuse, repetitive activities (e.g. computer use, racquet sports).