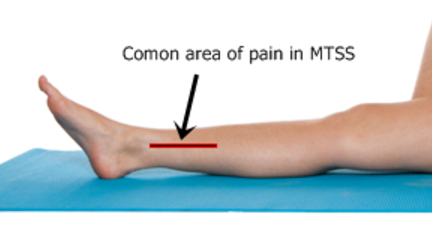
Is there an answer or should I toughen up and suffer in silence?
Preseason is a common time for overuse injuries and pain to present due to the sudden increases in training volume and intensity. Shin splints is one such injury, which seems to just get worse and worse. Often this problem plagues the athlete annually at this time of year. Occasionally it persists into the season to the point where the athlete is constantly playing through pain, suffering post-game and performances can begin to be affected. Since they haven’t had an “injury”, the athlete often feels like they just need to toughen up, push on through and it will pass. However, the problems seem to only get worse and worse the harder they push. Other athletes take time off and are increasingly frustrated to find the injury returns as soon as they get back to business.
So what is shin splints and what causes it?
Shin splints is actually a loose term because it encompasses a range of presentations, including stress fractures and compartment syndrome. It is still widely used but an attempt is being made to oust it. You may or may not have heard your physio refer to it as medial tibial stress syndrome. Medial tibial refers to the inside of the lower shin where symptoms are most frequently reported. Stress syndrome simply indicates that relative overuse is most commonly the cause.
As the narrowest part of the tibia, tiny bending movements occur at this site when running. This causes microscopic breakdown of the bone. There can also be breakdown of the connective tissue that encapsulates the deep muscles of the calf, where it attaches to the bone at this location. However, this is a normal process that occurs in everyone every time they go for a run. The strength of the original tissue and the amount and intensity of the running determines how much breakdown occurs.
Our bodies respond well and adapt to training. Our immune system will usually kick in pretty quickly to clean up the breakdown and lay down new bone and connective tissue in its place. As seen in the picture below, given proper loading volumes and recovery time, our bones overcompensate each time to get thicker, denser and stronger. This means that we can tolerate increasingly difficult challenges. This is a very similar process to how you can build muscle in the gym. However, bone does take a longer to recover, and longer to grow than muscle, but is just as plastic and adaptable.
From "How much is too much? (Part 1) International Olympic Council consensus statement on load in sport and injury risk" by Soligard et al. British Journal of Sports Medicine 2016: 50:1030.
How do I know how much is too much?
This varies greatly from person to person and is dependent of a number of factors.
Loading spikes:
We know that strong bones better resist breakdown and we know that bones get stronger over time. However, if you suddenly increase your training volume, frequency or intensity, you may not have time to sufficiently develop the bony adaptions necessary. Sometimes even changing mode of training to something very taxing on the calf muscles, such as hill running or skipping, is enough of overload the capacity of the tibia. Consistency and gradual increases in training load are imperative to avoid loading spikes.
Strength
Muscles develop at a different rate to bones. Importantly, muscle size is consistently associated with bone size and strength. This means bigger muscles are usually attached to stronger bones. Resistance exercises had been shown to increase bone density. Therefore, calf strengthening exercises can be useful in increasing the strength and size of the tibia so that less breakdown occurs.
Type of Runner
There are two extremes on a spectrum here. There is the athlete with calf and Achilles tendons like Pogo sticks. They often may be lacking in shock absorption and propulsion elsewhere. Naturally, if this is their primary source of power, it will also be the first area to overload. These athletes can often benefit from addressing the weaknesses elsewhere, reducing the demand on the calf muscles.
The other end of this spectrum is the athlete that has weak calf muscles, and is often knee dominant and heavy footed. A change in loading where calf strength is necessary can expose this weakness and cause overloading. Running retraining, and calf strengthening can work well in this population.
Nutrition and Bone Health:
Some people are genetically more vulnerable to low bone density. A family history of osteoporosis or stress fractures may hint at this as a factor. Another key issue is diet. We all know calcium is good for bones but vitamin D is also essential. Under-eating often occurs unintentionally, but when diet is compared with the massive energy requirements of greater than 5 sessions a week, calorie intake often becomes insufficient to meet energy expenditure. Nutrition is key to good bone health, and you can’t outrun a bad diet.
Pain Threshold
Pain is a protective mechanism, like a car theft alarm. It is designed to go off early and loudly before any substantial damage. This is a warning that there may be something to address. However, this threshold is very adjustable and dependent upon a multitude of factors. For example, the local nerve fibers become increasingly irritated and easier to set off when they are repeatedly overloaded. The red line in the picture above moves upwards and so it takes less to set it off. Like a car alarm that goes off in the middle of the night, it seems to get louder and louder.
We also know that lifestyle factors like getting poor sleep, feeling run down, stress, anxiety etc. can lower your overall pain threshold in the absence of pain or injury. In this instance, it takes much less breakdown to fire a pain response. Here, it is vital to address any of these factors that are modifiable to reconfigure the pain threshold to a more reasonable level.
Can the bone fracture?
The overwhelming majority of cases of medial tibial stress syndrome do not lead to stress fractures. This is because the rate of repair and breakdown usually meet an equilibrium long before the integrity of the bone is compromised. However, in some isolated incidences bone stress fractures can occur but this is rare. The pattern of pain with stress fractures is different from medial tibial stress syndrome. If you are concerned about developing a stress fracture, your physiotherapist can quickly establish the likelihood of it.
How do I know if I have medial tibial stress syndrome?
The common description of pain, is a dull diffuse ache along the inside of the shin. It will usually extend at least 5cm along the middle of bottom third of the shin. This pain comes on the beginning of exercise, but will often “warm up” and be less prominent as the exercise continues. As the local tissue becomes more irritated, it will last longer into exercise and may begin to even cause pain after exercise when walking or going up and down stairs. It is not limited to runners, and is very common in footie, soccer, hockey, netball and other field sports.
How long will it take to get better?
Compression garments, massage, dry needling, taping and shoe inserts may offer some short term relief. However, the results are mixed and often require trial-and-error to determine what works for that individual. They won’t solve the problem but can get you through the pain for long enough to successfully adapt.
There is great potential for long-term success the causing and contributing factors are identified and addressed. It can take time to build up the muscular, tendon and bone capacity. Likewise, the nervous system can take some time to cool down, especially the longer it has been wound up. Until then, a certain amount of patience is required. This carefully measured approach is the best way to ensure the problem doesn’t continue to spiral and progress.
What can I do for my shin pain?
1. Catch it as early as possible before it becomes increasingly irritated.
2. Start a training diary to get an idea of how much you are doing and how consistently you are training.
3. Address lifestyle factors if they are modifiable, such as diet, sleep and stress – obviously, this is not always possible!!
4. Visit a physiotherapist to identify your personal contributing factors and develop a management plan – there is no one-size-fits-all approach.